- Home
- About Us
- Treatments
- Testimonials
- Media
- International Patient
- Blog
- Cases
- Contact
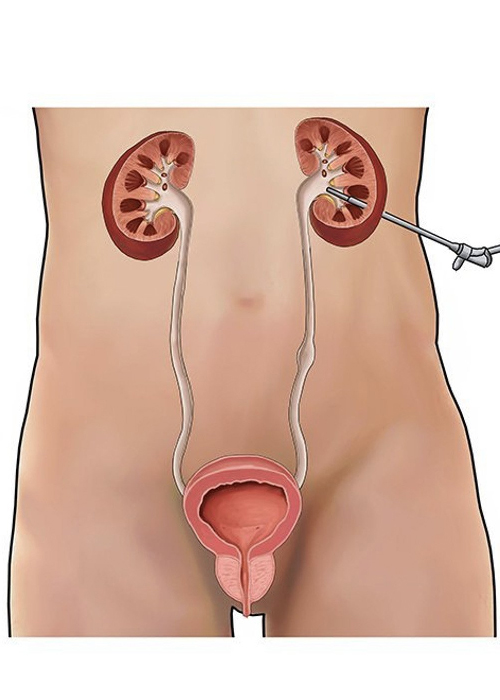
This leaflet explains more about percutaneous nephrolithotomy, a surgery to remove your kidney stones. It describes the benefits, risks, alternatives and what you can expect when you come to the hospital. If you have any further questions, please speak with a doctor or nurse caring for you. - Piles Doctor in Ahmedabad
A percutaneous nephrolithotomy (PCNL) is a procedure to remove a kidney stone or stones. Percutaneous means ‘through the skin’ and nephrolithotomy means ‘taking stones out of the kidney’. - Piles Doctor in Ahmedabad
From the results of your tests, your doctor has confirmed that you have a stone or stones in your kidney. Not all kidney stones cause symptoms, but yours may have caused significant problems, such as pain or infection. If nothing is done to remove them, they will continue to grow and could damage your kidney.
Problems relating to the anesthetic: such as a chest infection. More information about anesthetic and the risks associated with it is included in the leaflet Having an anesthetic. Please ask a member of staff for a copy. Problems relating to the surgery: deep vein thrombosis or DVT (blood clot in the legs), a pulmonary embolus (blood clot in the lung), stroke or heart attack. Bleeding: in or around the kidney. Some bleeding is normal; rarely it may be significant enough to require a blood transfusion (in less than five out of every 100 patients). If the bleeding does not stop, you may need an angiogram to block the blood vessel that is bleeding. This is a specialist treatment done in the x-ray department. In the rare event that this does not stop the bleeding, it might be necessary to remove the kidney (nephrectomy). This is extremely rare and happens in less than one out of every 1,000 patients. Infection: because some stones have bacteria trapped within them, we give you antibiotics routinely to prevent infection after the operation. A raised temperature is common after this procedure (25 out of every 100 patients), but this is usually temporary. One out of every 100 patients is at risk of sepsis (blood poisoning). Bowel perforation: there is a possibility of damaging the bowel during the operation. However, this is very rare and happens in approximately one out of every 500 patients (0.2%). Injury to the lung cavity: there is a small chance of pockets of air or fluids forming around a lung if the needle is inserted toward the upper portion of the kidney (this will have been decided by your surgeon depending on where the stones are). These pockets are treated with a chest tube, which allows the fluid to drain from around the lung. Fluid build-up: sometimes urine can leak from the kidney, resulting in a small collection of fluid inside the abdomen (tummy). If this becomes a large collection, it may need draining which is usually done in the x-ray department. In some cases, a temporary internal drainage tube called a stent is inserted. This is a small tube which runs from the kidney down to the bladder to make sure that the kidney is able to drain urine. Retained fragments: sometimes not all the stones are removed and these may need further treatment. Rarely, a stent is inserted during the procedure and left in place. If it has a string attached, it is removed within 24 to 48 hours; if it does not have a string attached, it can be removed within six weeks. An x-ray is taken before removing the stent to find out if the fragments have passed with the urine. - Piles Doctor in Ahmedabad
The consultant caring for you has recommended that a PCNL is the most suitable option for remove your stone(s). Possible alternatives include: extracorporeal shock wave lithotripsy (ESWL), and ureteroscopy (URS). A PCNL generally removes more stone fragments than ESWL and URS and has a shorter recovery time than open surgery. However, this will depend on your individual circumstances. Your consultant will discuss these options with you in more detail if they are appropriate for you. Please ask questions if you are uncertain. -Hernia Surgeon in Ahmedabad
We want to involve you in decisions about your care and treatment. If you decide to go ahead, you will be asked to sign a consent form. This states that you agree to have the treatment and you understand what it involves. If you would like more information about our consent process, please speak to a member of staff caring for you.
If you smoke, you will be asked to stop smoking, as this increases the risk of developing a chest infection or deep vein thrombosis (DVT). Smoking can also delay wound healing because it reduces the amount of oxygen that reaches the tissues in your body. If you would like to give up smoking, please speak to your nurse or call the Trust stop smoking service on 020 7188 0995, or call the NHS Smoking Helpline on 0300 123 1044. You will need to attend a pre-assessment appointment to assess your suitability and fitness for surgery and the anesthetic. This will also give you the opportunity to ask any further questions before you come into the hospital for the procedure. You must attend this appointment; if you do not, we may have to delay or cancel your surgery. Because of the risk of infection following stone surgery, if you have a urine infection before the operation the surgery will be postponed. If you think you have an infection while waiting for your surgery: give a urine sample to your GP. If the urine sample confirms infection, your GP will prescribe antibiotics. contact us as your surgery may need to be postponed to allow the infection to be cleared. If this happens, we will give you a new date for surgery.
If you are taking any medication, these may need to be temporarily stopped or adjusted around the time of your surgery or treatment, you will be given information on how to do this at your pre-assessment appointment. Do not make any changes to your usual medicines and continue to take them unless you have been advised to do so. Please remember to bring them to the hospital with you. If you are taking any medicines that thin your blood, such as antiplatelet medicines (for example aspirin or clopidogrel) or anticoagulant medicines (for examples warfarin or rivaroxaban), please tell your doctor or the nurse as you may need to stop them temporarily before your surgery. Also, tell your doctor or nurse if you have diabetes as you may need to alter the dose of your diabetes medicines, as you will need to fast before the procedure. Please let us know if you are taking any regular medicines (including anything you buy yourself over the counter or any herbal or homeopathic medicines) and if you have any allergies to any medicines. Further information on stopping any medicines will be given to you when you come for pre- assessment. Please ask us if you have any questions.
When you arrive at the ward, your admitting nurse will show you around. The nurses will also fill in any ward paperwork needed and carry out any tests that your consultant’s team has asked for. Even though you will have provided a urine specimen before, your urine will be tested again for infection, in case one has developed since then. If this is positive, your operation will probably be postponed. The evening before the surgery you will be given fluids and antibiotics into a vein to try to keep your kidneys working well and prevent infection. The evening or morning before your procedure, the anesthetic team will visit you and discuss with you the anesthetic they will use. You will be able to ask them any questions you have about your anesthetic at this time. On the morning of your surgery, you will be asked to have a shower and change into a theatre gown and elasticised stockings. These stockings help to reduce the possibility of clots (deep vein thrombosis or DVT) forming in your legs during surgery. These should be worn throughout your hospital stay.
Please do not eat or drink anything (except non-fizzy water) for six hours before your procedure. This means that you cannot suck on sweets or chew gum. You are allowed to drink water up to two hours before your procedure. If you continue to eat or drink after this, your surgery will be canceled.
This operation is carried out under general anesthetic, which means you will be asleep throughout the procedure. The operation begins by inserting a telescope-like instrument (known as a cystoscope) into the bladder. A tube is then passed up the ureter into the kidney. This tube allows the kidney to be filled with dye (contrast medium) which helps your surgeon to localize the kidney with x-rays. You are then moved into a prone position (lying face down). With the aid of the x-ray machine, the kidney is punctured with a fine needle. The needle position is confirmed by either outflow of urine or dye from the needle. Once the needle is positioned in the kidney, a 1.5cm incision (cut) is made in the back, and the needle tract into the kidney is stretched (dilated) to allow a telescope to be passed into the kidney. Other stone fragmentation tools such as a laser or an ultrasonic probe will also be inserted through this track for stone fragmentation and removal. The whole procedure usually takes two hours.
Once your procedure is over, you will be taken to the recovery room and remain there until you wake up from the anesthetic. This may take an hour or two. You will then be taken back to your ward. If you are in pain or feel nauseous (sick) while in the recovery room, please let the staff know. They can give you medicine to help with this. You will need to remain in bed at first. During this time, we will ask you to move your feet and ankles and wiggle your toes to help encourage circulation in your legs. This will also reduce the risk of blood clots in your legs. You will have a drainage tube from your kidney, which may be attached to a collection bag to drain your urine. The nurses will regularly empty the bag and measure the volume of urine produced. Try not to make sudden movements while the bag is attached. How long you need this tube depends on the number of leftover fragments, clots, and other debris. It is often removed the day after your surgery, but you may need x-rays to confirm when it is ready to be removed. You will also have a urethral catheter for the first 24 hours after your surgery. This is a tube inserted into the bladder through your urethra (a tube that carries urine from the bladder and out of the body). This may be uncomfortable; please tell us if it is so we can manage your discomfort. The average stay in hospital following this surgery is two to three days.
You may notice some blood in your urine for up to two weeks. Make sure you drink plenty of fluids to help with this. Aim to drink two liters (about three and a half pints or eight cups) of water, squash or fruit juice each day. We recommend that you do not drink more than two cups of tea or coffee each day. You should avoid drinking alcohol while you are recovering. You may feel sore around the operated area for several weeks; we will prescribe you painkillers to help with this. Avoid becoming constipated by eating a healthy, balanced diet, as straining to open your bowels increases the risk of bleeding. Eat plenty of fruit and vegetables and other foods high in fiber, such as wholemeal bread, pasta, and rice. If you need more advice about your diet, please speak to your doctor. Avoid lying down for long periods, as reduced movement increases the risk of developing pneumonia or blood clots in your legs. Avoid heavy lifting and straining for four weeks. Give yourself two to four weeks before returning to work. If your work involves heavy lifting or exercise, please speak to your consultant. Only start driving again when you are able to perform an emergency stop without feeling hesitant. Check with your insurance company to make sure you are covered to start driving again.
You will have a follow-up appointment six weeks after your procedure. On that day, you will have x-rays taken of your kidney and bladder. The consultant or a member of their team will continue to see you in future follow-up appointments.
Please contact the hospital if you experience any of the following after you have left the hospital: persistent bleeding or leaking of urine from the operation site fresh blood in your urine excessive pain a temperature of 38oC (100.4F) difficulty passing urine.

User visits the website and navigates to the "Appointment Booking" section.
After completing the form, the user submits their appointment request.
If the requested slot is available, the administrative staff confirms appointment.