- Home
- About Us
- Treatments
- Testimonials
- Media
- International Patient
- Blog
- Cases
- Contact
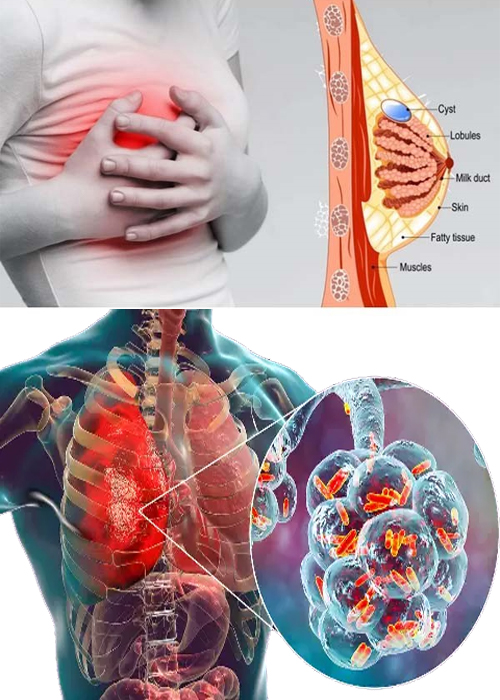
A benign breast condition is one that is not cancer. These problems often go away on their own or are easily treated. Because a few benign breast conditions can increase your risk of getting cancer in the future, you may Need to have follow-up tests or exams with your Breast Surgeon or other healthcare professional. Hernia Surgeon in Ahmedabad
Benign breast problems include pain, lumps or masses, infections, nipple discharge, and skin changes. Piles Doctor in Ahmedabad
There are two types of breast pain: 1) cyclic and 2) noncyclic. Cyclic breast pain occurs in response to changes in hormone levels. Your breasts may feel swollen, more sensitive, or painful before your menstrual period. You may have similar symptoms if you use combined hormonal contraception such as birth control pills or hormone therapy for menopause. Noncyclic breast pain is not related to the menstrual cycle. It usually occurs in one breast in one specific area. Many things can cause this type of pain, including injury, infection, medications, and large breast size. In rare cases, noncyclic breast pain can be caused by breast cancer - Piles Doctor in Ahmedabad
How is benign breast pain treated? For cyclic pain, wearing a well-fitted bra and taking pain-relieving medications can help. If you are on combined hormonal birth control, using your method continuously may improve symptoms. If you have noncyclic breast pain, see your ob-gyn or other healthcare professional. - Piles Doctor in Ahmedabad
There are different types of benign breast lumps. In general, benign breast masses are divided into three types:
This type of mass has normal cells. A common example is a cyst. Cysts are usually small. They usually go away by themselves or can be drained with a needle. Another example is a simple fibroadenoma. Simple fibroadenomas usually shrink or go away on their own. They may need to be surgically removed if they are large or keep growing.
In this type of breast mass, the cells are increasing in number but are otherwise normal. Having this type of lump slightly increases the risk of future breast cancer over the long term. They usually are surgically removed, but sometimes they can just be watched to make sure they are not growing.
Hyperplasia is a condition in which cells are increasing in number. Atypia means that the cells do not look normal under a microscope. Atypical hyperplasia greatly increases the risk of developing breast cancer in the future. Surgery to remove the cells and the area around them is recommended, along with close follow-up.
A common, benign breast lesion that presents as one or more solid lumps in the breast. Lump contain both connective tissue and tissue from the milk glands. Most often round and rubbery and will move around in the breast easily. Most often painless. Lump(s) can vary in size, anywhere from pea size to larger than a lemon. Who is prone to fibroadenoma? Fibroadenoma is more common in younger women in their teens and twenties. However, can occur at any age up until menopause. Fibroadenoma is responsive to hormone levels, therefore, women taking hormone therapy can get them even after menopause. Due to hormone-sensitive, fibroadenoma can change in size with varying hormone levels (i.e. during pregnancy, during the menstrual cycle). How is fibroadenoma diagnosed? A lump is first noticed during a self-breast exam or during a clinical breast exam with your healthcare provider. Further investigation with a mammogram and/or ultrasound is often recommended to rule out other breast diseases. Ultrasound (image below) is a useful tool as it can most accurately measure the size, determine the number and provide information on the growth of fibroadenoma over time. How is fibroadenoma treated? The treatment of a fibroadenoma depends on each patients’ needs, concerns and expectations. Most women monitor fibroadenoma through self-breast exams, clinical breast exam by their healthcare provider, and follow-up ultrasounds as determined by a radiologist. An ultrasound-guided core biopsy (see definition) may be recommended to rule out another breast disease. Surgery is not necessary unless the fibroadenoma is unacceptable to the patient, it continues to grow, or the diagnosis is questionable. Does a fibroadenoma put me at high risk for breast cancer? No. Fibroadenoma does not increase a woman’s risk of developing breast cancer in her lifetime. However, any new lump(s) found in the breast should be examined by your healthcare provider. What is mastitis? Mastitis is an infection of the breast tissue. It most commonly happens when a milk duct becomes clogged with milk during breastfeeding and does not drain properly. Your breast will be red, swollen, warm, and painful in one specific area. Mastitis can cause flu-like symptoms, such as fever, aches, and fatigue. How is mastitis treated? You may be prescribed an antibiotic to treat the infection. Applying warm compresses can help relieve the pain. It is safe to breastfeed your baby when you have mastitis and are taking an antibiotic. What are the signs and symptoms of nipple discharge? Benign discharge tends to occur in both breasts and only when the breast or nipple is squeezed. It is usually milky white or greenish in color. Discharge that is bloody or clear is more concerning. What causes nipple discharge? Discharge from the nipple is a common benign breast symptom. During pregnancy, nipple discharge is normal as the breasts get ready to produce milk. In women who are not pregnant, it can be caused by hormonal changes. Some medications can cause nipple discharge. Nipple discharge should be checked by an ob-gyn or other healthcare professional. What skin changes can affect the breasts? Breast skin can be affected by common skin problems, such as psoriasis and eczema. Yeast infection of the skin folds under the breast is a common condition. Women with large breasts are more likely to have this problem. Some skin changes of the breast raise concern for cancer. These include redness, warmth, dimpling of the skin, and ulcers (small, red, painful blisters). Nipple changes such as crusting, scaling, or a nipple that has changed shape also raise concern. Tell your ob-gyn or other health care professional about any skin changes that you notice. How are benign breast conditions evaluated? If you have breast symptoms, let your healthcare professional know. You most likely will have a breast exam. In some cases, you may need to have an imaging test of your breast. Breast imaging can be done with mammography, an ultrasound exam, or magnetic resonance imaging (MRI). Imaging may be followed by a biopsy. What kind of follow-up will I need if I have a benign breast condition? Most benign breast conditions do not increase your risk of cancer, but some, such as certain types of breast lumps, do. If you have a condition that increases the risk of cancer, more frequent clinical breast exams and imaging tests over the next 1–2 years may be recommended. The recommended course of follow-up is based on your age, health risks, and test results. What is breast self-awareness? Being aware of how your breasts normally look and feel is called breast self-awareness. Knowing what is normal for you will help you detect any changes that may signal a problem. If you notice any of the following, contact your health care professional: A new lump Skin changes —Thickening —Dimpling —Unexplained reddening —Nipple scaling or redness —Ulcers Pain (especially if it is in one place or is getting worse)

User visits the website and navigates to the "Appointment Booking" section.
After completing the form, the user submits their appointment request.
If the requested slot is available, the administrative staff confirms appointment.